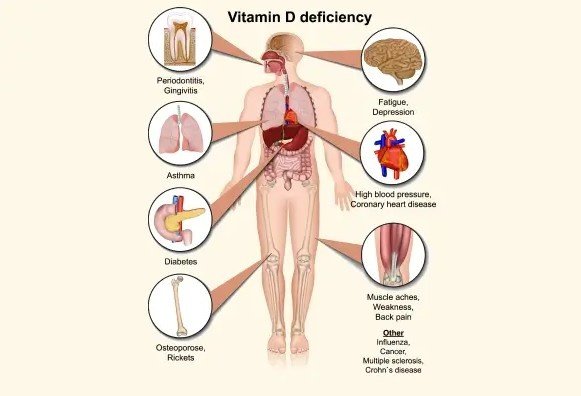
Vitamin D plays a crucial role in maintaining bone strength, muscle function, and overall health. Despite its importance, Vitamin D deficiency has become increasingly common due to lifestyle changes, limited sun exposure, and dietary habits. Early diagnosis is essential to prevent complications such as weak bones, joint pain, and fatigue. Patients seeking the Best Vitamin D Deficiency Treatment in DLF Phase often begin with a detailed diagnostic process that helps identify the severity of deficiency and its underlying causes.
For fast information, contact us on WhatsApp.
At Ortho Plus Care, the focus is on accurate diagnosis and personalized care. The Best Vitamin D Deficiency Treatment in DLF Phase involves a systematic evaluation of symptoms, medical history, and laboratory tests to ensure effective treatment planning. Understanding how diagnosis is carried out can help patients take timely steps toward improving their health.
Understanding Vitamin D Deficiency
Vitamin D deficiency occurs when the body does not have enough Vitamin D to maintain proper calcium absorption and bone health. This deficiency can affect individuals of all age groups.
Patients consulting for the Best Vitamin D Deficiency Treatment in DLF Phase may experience symptoms such as bone pain, muscle weakness, fatigue, or frequent infections. In some cases, the deficiency may remain unnoticed until it leads to more serious complications.
Early detection is important because untreated deficiency can contribute to conditions like osteoporosis or reduced bone density.
Importance of Early Diagnosis
Timely diagnosis plays a key role in preventing long-term health issues. The Best Vitamin D Deficiency Treatment in DLF Phase begins with identifying symptoms and confirming the deficiency through medical evaluation.
Many individuals ignore early signs such as fatigue or mild joint pain, which may delay diagnosis. Consulting a specialist at the right time helps prevent the progression of symptoms.
Early diagnosis also allows doctors to recommend appropriate treatment before complications arise.
Clinical Evaluation by Specialists
The first step in diagnosis involves a detailed clinical evaluation. The Best Vitamin D Deficiency Treatment in DLF Phase includes assessing the patient’s symptoms, lifestyle habits, and overall health condition.
Doctors at Ortho Plus Care examine factors such as sun exposure, dietary intake, and medical history. These factors help determine whether a patient is at risk of Vitamin D deficiency.
A comprehensive clinical assessment provides valuable insights that guide further diagnostic testing.

Blood Tests for Accurate Diagnosis
Blood testing is the most reliable method for diagnosing Vitamin D deficiency. The Best Vitamin D Deficiency Treatment in DLF Phase includes measuring serum 25-hydroxyvitamin D levels in the blood.
This test helps determine whether Vitamin D levels are sufficient, insufficient, or deficient. Based on the results, doctors can assess the severity of the condition.
Accurate blood test results are essential for creating an effective treatment plan tailored to the patient’s needs.
Evaluating Bone Health
Vitamin D deficiency can significantly impact bone health. The Best Vitamin D Deficiency Treatment in DLF Phase may include evaluating bone density and strength, especially in patients experiencing bone pain or fractures.
In some cases, imaging studies or bone density scans are recommended to assess the condition of bones. These tests help identify early signs of bone weakening or osteoporosis.
Monitoring bone health is an important aspect of diagnosing and managing Vitamin D deficiency.
Identifying Underlying Causes
Vitamin D deficiency can occur due to various reasons, including limited sun exposure, dietary insufficiency, or certain medical conditions. The Best Vitamin D Deficiency Treatment in DLF Phase focuses on identifying these underlying causes.
Doctors may evaluate factors such as digestive health, kidney function, and medication use to determine the reason for deficiency. Understanding the root cause helps ensure that treatment addresses the problem effectively.
This approach reduces the chances of recurrence and supports long-term health improvement.
Assessing Lifestyle and Risk Factors
Lifestyle habits play a significant role in Vitamin D levels. The Best Vitamin D Deficiency Treatment in DLF Phase includes assessing daily routines, outdoor activities, and dietary patterns.
Individuals who spend most of their time indoors or have limited exposure to sunlight may be at higher risk. Similarly, inadequate intake of Vitamin D-rich foods can contribute to deficiency.
Evaluating these factors helps doctors provide recommendations that support both treatment and prevention.
Personalized Diagnosis and Treatment Planning
Every patient’s condition is unique, and diagnosis must be tailored accordingly. The Best Vitamin D Deficiency Treatment in DLF Phase involves creating a personalized plan based on test results and individual health needs.
Doctors consider factors such as age, existing medical conditions, and severity of deficiency when planning treatment. This personalized approach ensures that patients receive the most appropriate care.
Customized treatment plans improve the effectiveness of therapy and enhance recovery outcomes.

Monitoring Progress After Diagnosis
Diagnosis is not a one-time process. Continuous monitoring is essential to track progress and adjust treatment if needed. The Best Vitamin D Deficiency Treatment in DLF Phase includes follow-up tests to evaluate improvements in Vitamin D levels.
Regular monitoring helps ensure that treatment is working effectively and allows doctors to make necessary adjustments. It also helps prevent the recurrence of deficiency.
Ongoing care plays a key role in maintaining optimal health.
Role of Preventive Care
Preventing Vitamin D deficiency is just as important as treating it. The Best Vitamin D Deficiency Treatment in DLF Phase emphasizes preventive measures such as maintaining a balanced diet and ensuring adequate sunlight exposure.
Patients are guided on lifestyle changes that support healthy Vitamin D levels. These may include incorporating Vitamin D-rich foods and maintaining regular outdoor activity.
Preventive care helps reduce the risk of future deficiencies and supports overall well-being.
Conclusion
Vitamin D deficiency is a common yet manageable condition when diagnosed early and treated appropriately. A structured diagnostic process helps identify the severity of deficiency and its underlying causes, allowing for effective treatment planning.
The Best Vitamin D Deficiency Treatment in DLF Phase at Ortho Plus Care focuses on accurate diagnosis through clinical evaluation, blood tests, and assessment of lifestyle factors. With personalized care and continuous monitoring, patients can improve their Vitamin D levels and maintain better bone and overall health.